If you’re one of the 70 million Americans suffering from obesity and are tired of diets and exercise that don’t work, you should consider gastric sleeve surgery. Laparoscopic sleeve gastrectomy is one of the safest and most effective methods of weight loss surgery. A 2011 study of 2,400 patients revealed that gastric sleeve surgery had much lower complication rates and reoperation rates than Lap Band surgery.
However, even though a gastric sleeve is just as safe as some of the most minor abdominal operations, it is still surgery and like all surgeries can have certain risks and complications associated with it. Here we’ll look at some of the reported gastric sleeve complications and how you can address them so you can make a well-informed decision about what is best for you.
What Is Gastric Sleeve Surgery?
A gastric sleeve procedure, also known as sleeve gastrectomy, is where a bariatric surgeon removes about 75% of your stomach; leaving you with a long, narrow, new ‘sleeve-like’ or ‘sleeve-shaped’ stomach that is about the same diameter as your index finger. With much less room for food in your stomach, you’ll feel full faster, you won’t be able to eat as much as you used to eat, and your body won’t produce as much of ghrelin, the ‘hunger hormone.’ All of that will likely add up to you losing a lot of weight through gastric sleeve surgery.
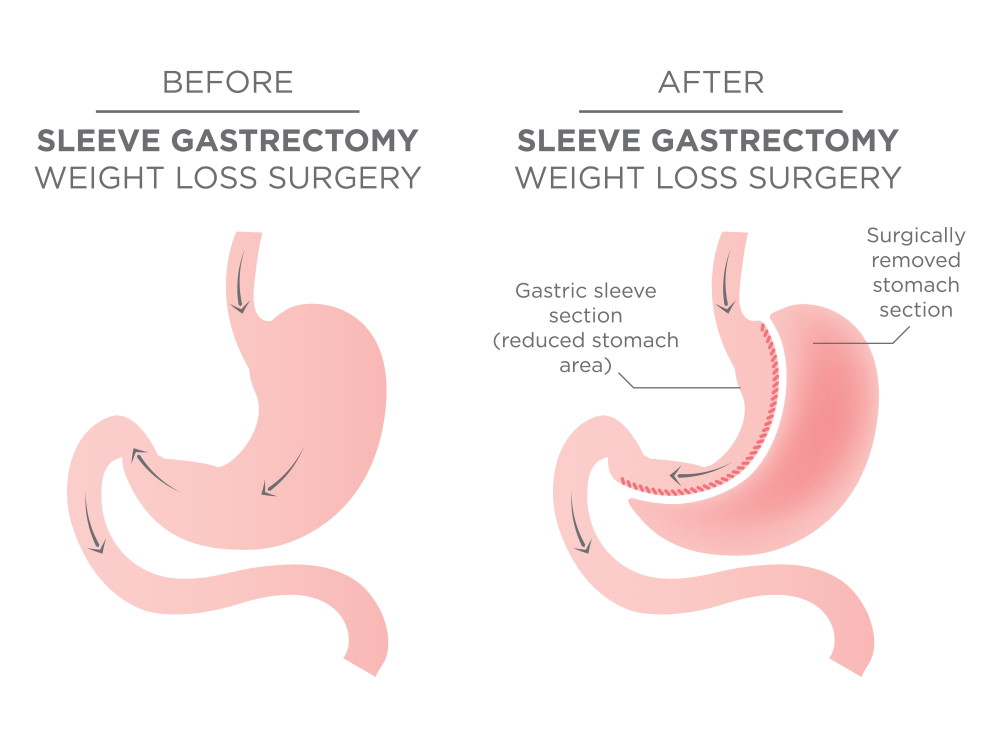
The gastric sleeve surgery takes about 30 minutes to complete. The bariatric surgeon will make very tiny incisions in your skin and insert an instrument with a tiny camera that projects images onto a screen called a laparoscope. Laparoscopic and robotic gastric sleeve surgery is less invasive than open weight loss surgery. Next, the surgeon will use other medical instruments to remove part of the stomach and connect the rest of it to form the ‘sleeve.’
Some patients will stay in the hospital overnight, but if doing well some will be able to go home safely the same day once they are consuming clear liquids consistently. The operation is permanent. Once you leave the hospital, your diet will consist of protein shakes and blended foods for the first four weeks. You’ll slowly phase into soft solid foods, and after about six weeks, you’ll be able to move on to regular meals, chewing slowly and eating much less than you used to.
What Are The Potential Complications With Gastric Sleeve Surgery?
Gastric sleeve surgery is a safe and efficient way to lose weight. While this bariatric procedure isn’t as established in the medical community as other weight loss surgeries, it is quickly becoming one of the most sought after.
While the procedure is usually perfectly safe, there are some possible risks and potential complications that could occur. It’s important to be aware that every type of surgery does carry potential risks, even minor outpatient procedures. It’s vital to discuss the risks, benefits and even alternatives of the gastric sleeve surgery with your bariatric surgeon before you commit to the procedure.
Here we break the most common reported gastric sleeve complications down into two categories: short-term and long-term.
Short-Term Complications
Within the first two weeks of your gastric sleeve, you will still be adjusting to your new life. This stage can be hard because your diet will be pureed food, protein shakes, and water. You might feel moody or depressed. The incision sites may still be a bit tender. It is important to know that the most serious complications of gastric sleeve surgery can occur during this period. Although complication rates are overall low, it’s important to understand the risks.
Dehydration
By far the most common early gastric sleeve complication is dehydration. Following surgery, patients should be given very clear hydration instructions. However, following surgery, patients can only tolerate very small amounts of fluid at a time due to sleeve swelling. So for the first two to three weeks following surgery they will need to place a full-time focus on continuous sipping to avoid dehydration. When patients get distracted, dehydration often results. The most common symptoms of dehydration are listed below:
- Nausea
- Constipation
- Back aches and muscle cramps
- Low urinary output
- Concentrated dark urine
- Dizziness
Unfortunately, because nausea is one of the common early symptoms, this can make it even harder to catch up on hydration and sometimes lead to even worsened dehydration. Because of this it is very important to follow your surgeon’s recommendations, using constant sipping for the first two weeks following surgery. If dehydration becomes very severe, doctors may need to prescribe nausea medication; and in some cases a patient may even need to be rescued with IV fluids. In almost every case dehydration can be prevented by consistently following post-op instructions, and so it is very important to plan to take at least two weeks off of work as you recover and intentionally avoid all distractions so that you can avoid experiencing dehydration.
Staple Line Leaks
A rare yet potentially serious gastric sleeve complication is a staple line leak. When this problem occurs it will usually be within the 7 to 10 days after surgery. It involves the staples the surgeon uses to close a patient’s stomach being disrupted or opening up, resulting in fluid leaking out of the stomach into the intra-abdominal space around the stomach. A staple line leak complication may manifest in the following ways:
- Fever
- Fast heartbeat
- Difficulty breathing
- Lightheadedness or dizziness
- Severe abdominal pain
If patients experience these symptoms, it is very important to call their surgeon immediately. If the leak is contained, sometimes surgery can be avoided using stents and other supportive treatments. If, however, the leak is not contained, a repeat operation to find and repair the leak may be required.
According to most national data this is a very rare problem affecting less than 0.5-1% of patients after gastric sleeve surgery. Preventing this complication starts long before surgery by eliminating harmful substances to the stomach such as nicotine. Then during surgery an intra-operative leak test is performed to make sure that the staple line is airtight without any leaks before the patient leaves the operating room. Finally, the patient needs to be very careful to follow the surgeon’s post-operative protocols in detail and consistently to minimize the risk of traumatizing the airtight staple line.
Infection Around Incision Site
Another complication of gastric sleeve surgery is an infection around one of the incision sites. In the era of minimally invasive surgery, this also very rare; occurring in less than 1% of surgical cases. While infections can occur after any surgery, obesity does raise this risk slightly. Symptoms of a wound infection can include:
- Fever
- Redness and heat around the incision site
- Puss coming from the incision site
To treat the infection, sutures may need to be removed to wash out the wound site. Topical antibiotic or antimicrobial ointments may be applied, and depending on the wound antibiotics are sometimes prescribed. Fortunately, careful precautions (including good preoperative hygiene with a shower the evening before and morning of surgery, preventative antibiotics around the time of surgery, a sterile surgical prep, and very small minimally invasive incisions) make a wound infection very unlikely following sleeve gastrectomy surgery.
Stricture
Another very rare complication after gastric sleeve surgery is the abnormal formation of scar tissue around the sleeve, creating a blockage in the stomach that prevents food from passing through. This condition is called a stricture. It can either occur early after surgery or it can present in a more delayed fashion. A patient should contact their doctor if they experience these symptoms:
- Nausea and vomiting directly after eating
- Difficulty swallowing
- Onset of intolerance to solid food
- Severe heartburn
If detected shortly after surgery, this can sometimes be due to very tight swelling rather than scar tissue and is usually treated with rest and intravenous fluids and nutrition if needed. If more than three weeks have passed without resolution of the stricture on radiology images, the doctor may then need to perform an endoscopic dilation to open the stricture. If several dilations do not resolve this problem (which is very rare), then surgery may be required.
Blood Clots
Blood clots, known as deep venous thrombosis, are also a rare potential complication of sleeve gastrectomy surgery that occur in <1% of patients nationally. At the BMCC we understand these risks and have detailed protocols specifically designed to mitigate them. Blood clots are most likely to form during the surgery recovery period, especially when patients are not standing and walking. Symptoms usually occur around the arms or legs and can include:
- Asymmetric extremity swelling
- Pain in the extremity
- Chest pain (if the clot travels to the lung)
- Sudden shortness of breath (if the clot travels to the lung)
Blood clot treatment is usually limited to treatment with blood thinners to dissolve the clot.
Long-Term Complications
These complications can be either acute or ongoing. Although these complications aren’t serious, they can be persistent and cause a lot of discomfort nonetheless.
Heartburn
Heartburn, or gastroesophageal reflux disease (GERD), is the most common long-term complication after sleeve gastrectomy or any weight loss surgery. Up to 20% of the patients who undergo gastric sleeve surgery in one study experienced increased heartburn after their sleeve. If this occurs it’s treated with proton pump inhibitors and antacids. Very rarely surgery may be required if medications are not effective and severe symptoms persist beyond a year after surgery.
Deficiencies
Compared to gastric bypass surgery and loop duodenal switch surgery, nutritional deficiencies are much less common for patients who undergo sleeve gastrectomy surgery. This is especially true for patients that are consistent with taking all recommended vitamins and keeping up with recommended protein intake after the procedure. If vitamin deficiency occurs, common signs include ashen skin, hair loss, fatigue, dizziness, and constipation, among others. Your doctor will instruct you to take vitamin supplements regularly to avoid this issue.
Gallstones
Up to 15% of gastric sleeve patients can experience gallstones that are precipitated by their weight loss during the first year after surgery. Symptoms can include severe pains in the upper abdomen and back as well as nausea and vomiting. These symptoms are often exacerbated by fatty meals. At the BMCC we utilize a medication that dissolves gallstones as they are trying to form to prevent most patients from developing gallstones during their weight loss period. For the rare patients that still develop gallstones, they are then treated with a simple minimally invasive day-surgery to remove the gallbladder.
Do The Benefits Outweigh The Risks?
While there are risks associated with the sleeve gastrectomy, the overall risk of experiencing major complications is no higher than with the most minor abdominal surgeries. Ultimately surgery is a life-changing procedure whose advantages far outweigh the risks.
When compared to other weight loss surgeries, this surgery is simpler and more straightforward than gastric bypass, often meaning less chance of surgical complications. Gastric sleeves also don’t cause dumping syndrome as frequently as gastric bypass surgery does or require adjustments or organ rearranging.
While it is true that some risks rarely can occur following gastric sleeve surgery, the risks of obesity are far greater. In fact, the gastric sleeve (like most other forms of bariatric surgery) has been shown to prevent or decrease risk for most of the top causes for death in the US including heart disease, cancer, respiratory diseases, stroke, and diabetes; leading to a significant reduction in the risk for early death. But just as important as preventing early death and lengthening your life, the gastric sleeve also gives you an opportunity to live… to live the much higher quality, richer, and more fulfilling life that you deserve to live.
The Bariatric and Metabolic Center of Colorado Is Right In Your Neighborhood
Dr. Joshua Long has made a lifelong commitment to helping people like you lose weight and live better, healthier lives. He takes a personal engaged approach to each and every patient to find out what makes them unique. This helps him and his team develop a customized and comprehensive treatment plan no matter what stage you are in your journey. This personalized method reduces complication rates and increases successful weight loss. Dr. Long’s perfectionism has earned several awards, distinctions, and prestigious designations.
To find out more about this life-saving weight loss procedure, schedule an appointment with our friendly office staff.
